My first son's birth was an amazing, empowering home birth, and I wrote that story as the final chapter to my first memoir.
My second son's birth was a tragic, traumatizing stillbirth by cesarean that nearly killed me. I wrote about it here: Gifts Hidden In Loss
Rainbow babies are the little miracles that help grieving parents heal our hearts and find hope and beauty after the storms of miscarriage and stillbirth. The whole pregnancy of a rainbow baby is marred by fear, stress, and grief. Fear we'll lose this one too. Stress because the pregnancy is treated as high-risk, requiring frequent monitoring, especially the last month. Grief as every little thing brings up our only memories of the lost babies, and what we wish we'd done differently, what we would have done if only we'd known, questioning if we could have done something to save the losses...
My pregnancy with Dylan was so different from my first two, I was positive I would have a girl. I had severe food aversions (didn't want to eat at all,) all day nausea for 20 or so weeks, lost 20 pounds instead of gaining, fainted once in the first trimester and once in the second, all things I had never experienced before.
This was also my first planned pregnancy, with a husband and a mother in law interested in the baby and supporting me. My mother in law was with me and my oldest when we finally got the sonogram that looked for genitalia. "I KNEW it'd have a penis!" My son, Aiden, shouted triumphantly.
The pregnancy was high risk for many reasons. I was considered old (36,) morbidly obese, I developed gestational diabetes that required metformin and insulin to bring down the fasting blood sugar (though I easily managed the after meal sugars with diet and exercise,) my previous pregnancy had been a 13 pound 12.4 oz stillbirth at 42 weeks, I'd had a Cesarean, I'd hemorrhaged afterward and had to have 5 units of blood (wrote about that here: Dead & Back Again: This Mama's Experience,) and there may have been another couple of risk factors that I no longer remember.
I was terrified of hospital birth, especially after my experience with my second son, but once I required metformin, I risked out of the birth center I'd hoped to have a home birth with. It was so late in the game, I was stuck with a high risk practice I didn't like. There were 27 doctors in the practice, all surgeons, and I saw a different one almost every visit. They all told me different things, and the language they used when I told them I wanted a VBAC (vaginal birth after Cesarean) made me feel that they had no interest in or faith in my doing so.
Because of the diabetes, they demanded I deliver my son at 39 weeks even though I was doing an excellent job keeping my blood sugar under control and had no problem symptoms at all. Even though I'd been testing my urine for ovulation and the dating scan we got initially showed my son should have been due on July 6th 2017, they went by the date of my last period, saying he was due July 1st. That worried me. I didn't want him born too soon. I was afraid that might cause nursing problems (it did,) or worse, he might end up in the NICU (he didn't, thank goodness.)
Several of the doctors of that high risk practice told me they would allow me to try to labor after Cesarean (TOLAC,) and that they would attempt to induce vaginal labor at my request. Come to find out, they lied. More on that in a moment.
I had a lot of love and support this pregnancy, unlike the last two. I had two doulas who are both good friends of mine and helpful in different ways. One, Sheri, is an accupuncturist, and she gave me lots of great practical advice and stayed on top of me so I wouldn't forget to take it. She recommended two books that helped me calm down and plan for the best hospital birth experience, Natural Hospital Birth and Homebirth In the Hospital. I wouldn't have gotten to have Dylan vaginally if it hadn't been for her. The other, Michelle, is a hypnotherapist and a bereavement doula who was there in the hospital with me when I lost Galen. She taught me Hypnobirthing and used her magic voice to help me through the worst parts of both births.
The high risk practice I got stuck with only delivered with the hospital in Orlando with the worst Cesarean rate. I didn't feel safe there. I wanted to deliver my son at a new, very VBAC-friendly hospital closer to my house, at which I preregistered weeks before my "induction" was scheduled. So the day before the scheduled induction, Sheri suggested I go to the hospital of my choice and get checked to see if I was dilated enough to deliver there.
At 9pm that night I went in to get checked out. I told the midwife there my story, and she requested my paperwork from the other hospital. She told me that I had been scheduled for a repeat Cesarean at the other hospital, and showed the order to me.
I was livid that the doctors had lied to my face, and terrified of going in for a repeat surgery the next morning, as every Cesarean is risky, and the more you have, the more risks. Laboring mothers in America die more than in most other developed nations in part because of our outrageously high Cesarean rates, and my first Cesarean almost killed me. I also knew that I would recover faster from a vaginal birth, and I couldn't imagine taking care of my newborn and trying to breastfeed while recovering from major surgery. I know a lot of women do, but I don't think anyone would choose to if they knew from previous experience that uncomplicated vaginal birth was so much gentler and easier to heal from, as I did.
I thought they were going to send me home, because when the midwife checked me I was barely dilated at all. I cried my heart out for about 40 minutes. I didn't know what to do. (So I posted to Facebook and got some comfort and advice.)
Then an OB came in and told me they would be happy to keep me and induce me, if I really wanted to try for a VBAC. I did! I did! After he left, I cried happy tears. (And posted to Facebook. I chronicled the whole journey there until I couldn't anymore. Looking forward to seeing my "On this day" posts next year!)
They admitted me at 3am, but didn't start the induction with the bulb until 7am. The schedule changed then, so I ended up with a different doctor and different nurses. Basically, they put a balloon in my cervix and filled it at both ends with saline so it would manually stretch out my cervix. 12 hours later, it still hadn't fallen out on its own, but it had opened me up to about 4cm. Then we started the low dose of pitocin. More on that in a minute.
If you live in Orlando and have to give birth in a hospital, I HIGHLY recommend Florida Hospital For Women. Every single nurse, doctor, and midwife I saw during my induced labor took the time to read my birth plan, talk to me about my story, and they followed it as much as possible. I was amazed and impressed and rave about them to anyone who will listen.
I had an amazing birth plan. Michelle asked if she could copy it to show her future clients. And like the best laid plans, pretty much nothing went according to it...lol
So back to the pitocin. The low dose got contractions going off and on. 12 hours later I was still at 4cm. New doctor shift, new plan. I took an hour with my husband and son to give my body a break from the pitocin and my poor butt a break from the bed. I'd been pretty much stuck in the bed because my big belly flipped the baby monitor every time I moved, and once we started the pitocin he had to be constantly monitored for his safety. My sacrum was in agony about an hour in. There was no comfortable position. I could just shift pressure from one side to another. So the goal was to get me dilated enough to break my water, and then put on internal monitoring. Once the internal monitor would be put it, I would be able to use the birth ball and walk around and do other natural things to get my baby moving down and my labor progressing.
We started another round of pitocin, and the labor really started. It was unpleasant, but with my hypnobirthing training, I was okay. But it was the slowest labor of all time. I'd thought when they put the bulb in that I would have my baby within 12 hours. I'd texted everyone to let them know to expect to come to the hospital soon. My sister of the heart, Niki, and her daughter, Beth, wanted to be there and had a 2.5 hour drive, my husband's mother had a 4 hour drive, and we all thought my labor would go super fast after my water broke, because my first son was delivered 5 hours after my water broke and my second son, I had gotten to 9cm 3 hours after my water broke.
Niki and Beth ended up coming up, spending several hours with me, then going back home when my labor didn't progress, as they both had to work. I had more pitocin overnight, and the next morning the doctor on shift decided I was open enough to break my water. So he did, immediately, and immediately put in the internal monitors.
YAY! FINALLY! Now I could use the birth ball and walk and get off my poor butt!
Except I stood up to use the bathroom and my baby's heart rate decelerated from the 150s to the 40s.
A bunch of nurses rushed in and basically threw me on the bed, gave me oxygen and had me roll to my side. His heartbeat stabilized, and I would not be allowed out of the bed again until after he was born. I had to pee in a bedpan, which was not my favorite.
At that point I had still been hoping for as natural a birth as possible. I didn't want an epidural because I'd gotten one at my Cesarean and it hurt and scared me, and it hadn't even fully worked. I planned to use hypnobirthing and getting into the birth trance I'd gotten into with my first son's home birth.
Sheri came that morning, but had to leave to take care of her son before I had my baby, sadly. I was sorry she missed it, and grateful she was able to do what she did. Michelle arrived sometime before Sheri left, and she stayed the rest of the time.
We started the next round of pitocin after breaking my water, and I started wondering if an epidural might be okay after all. Pitocin-induced contractions give you all the pain and none of the endorphins that natural contractions with natural oxytocin provide. At one point, Michelle used her magic voice to get me in that trance I remembered, and I knew that if I kicked everyone else out and just had Michelle talk me through the contractions, I could get through the rest of my labor without needing an epidural.
But I didn't want to kick everyone else out. I wanted my son and husband and mother in law to get to see Dylan be born. I wanted Michelle, Mackenzie, Niki and Beth, who had all been at Galen's birth, to have the closure and the pleasure of being a part of my rainbow baby's birth. And I wanted them all with me, for me. When I reached 6cm, I had a contraction that was a 9 out of 10 on the pain scale, and I knew they were going to be 10s soon. Soon the pain would be just about unbearable. I realized that there was nothing natural about this birth, and that was okay. So I asked for an epidural.
Getting the epidural was the absolute worst part of the birth.
It doesn't have to be, I've heard. But both times I've gotten an epidural were traumatic. The first time I was in agony, grieving, and had contractions 45 seconds apart, but they got it in pretty quick. This time they were apparently training someone. They talked casually about it, saying, "crunch crunch crunch" as they were pushing the needle through something in my spine that crunched, and it hurt, and it was scary. It took an hour for them to finally get it in, on the fourth try, and I had a panic attack or a PTSD flashback about 30 minutes in and cried while Michelle soothed me. I was too wrung out to feel relieved when it was over, but when it started working I was SO glad I'd gone with it. After three days of constant pain in my sacrum, I finally had relief, and got a little sleep. I was able to fully relax, and with the hypnobirthing training I'd done, I mean FULLY relax.
And it still took FOREVER to dilate all the way. I think it was another twelve hours. I had time to share my life story and everything I knew about natural birth with an unsuspecting student doctor. That was just before they finally checked me and felt the baby's head instead of my cervix. I'd been shaking the whole time I was talking to the student doctor, and I think I was ready to push before he even came in. But the epidural worked so well, I couldn't feel pretty much anything. The midwife and doctor and nurses had all told me to tell them if I felt like i needed to poop, as that would be the baby's head moving, but the sensation was so mild I was never sure I was feeling it, so I didn't say anything.
The midwife I'd seen the very first night ended up being the midwife who caught my baby. They got me into position, Niki ran to fetch my husband, son, and mother in law, and as they walked back into the room, Dylan slid out on the second push, like butter. I was so relaxed there was no tearing, no soreness at all in my birth canal or surrounding areas even immediately after the epidural wore off.
That picture of them up top, the expressions on their faces as they saw Dylan being born, melts my heart.
I checked in 9pm Friday, and birthed Dylan 8pm Monday. Very little of the birth went according to plan or expectation, but it was still beautiful, peaceful. I felt respected and supported the entire time, and just so grateful to have doctors that didn't try to rush me into surgery for "failure to progress" even 13 hours after breaking my water.
I only wish I could have seen him slide out!




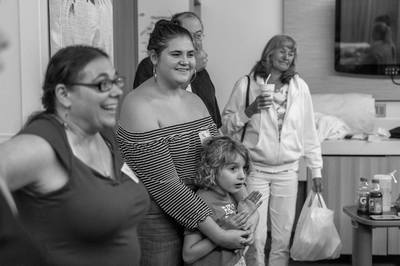

 RSS Feed
RSS Feed
